News

Hands-On MIS 2026 — Pediatric & Neonatal Workshop
Udaipur
February 2026Wonderful few days conducting a hands-on workshop in Udaipur for the Rajasthan Association of Pediatric Surgeons and IAPS Chapter of Rajasthan. It involved sharing, learning, teaching, and operating together at the Hands-On MIS Workshop in Udaipur.
Nothing is more fulfilling than seeing young surgeons grow confident with new skills that will help children for years to come.
At Medical College & Hospital, the Hands-On MIS 2026 workshop brought together faculty, trainees, and pediatric surgeons with a shared objective — advancing minimally invasive surgery for children through direct mentorship, live operating room teaching, and collaborative learning.
Over several intensive days, the workshop combined:
- Live operative demonstrations
- Interactive case-based discussions
- Dry-lab and video training sessions
- Real-time surgical decision-making in pediatric and neonatal cases
More importantly, the atmosphere reflected something deeper: capacity building — empowering local teams with techniques that improve recovery, reduce pain, and expand access to advanced pediatric surgical care.

Casual Conversation Leads to History-Making Surgery
Chaitanya Deshpande
April 29, 2019A passing conversation between doctors in the surgical lounge at MU Health Care’s Women’s and Children’s Hospital ultimately led to a history-making procedure halfway around the world in India.
“He was talking about his mission trip,” An said. “I told him it sounded amazing and asked if I could go with him next time.”
Pimpalwar had never taken an ophthalmologist with his team in the past, so he invited An to join him for the week-long February mission to Manipal and Mangalore in the southwestern part of India.
But An didn’t want to just share her expertise with doctors overseas. She wanted to give them something they could use long after she had gone.
“I was thinking, ‘How can I make this sustainable?’ Not just show them what I do, but give them something they can do.”
An is a fellowship-trained surgeon in micro-invasive glaucoma surgery (MIGS), a procedure that decreases pressure in the eye to prevent vision loss. An wanted to bring that technique to her counterparts in India, complete with all of the tools to perform the surgery. She reached out to New World Medical’s humanitarian charitable product donation program. They agreed to supply more than $34,000 worth of blades and devices to support MIGS and tube implant procedures. An received the supplies just days before the trip.
“Everything happened very quickly, and then I packed up and went,” An said.
Once in India, An realized she had a lot of teaching to do – a learning curve to overcome in just one week’s time. She worked with the doctors at Kasturba Hospital in Manipal to help them determine which types of patients would be most appropriate for different MIGS and tube procedures, then led them through pre-op, surgery and post-op management. They worked 13 cases together.
“I gave a lecture and a wet lab session every day on a different topic,” An said. “Surrounding hospitals started to hear about me, and they invited me for an ophthalmology conference, where I delivered a lecture on micro-invasive glaucoma surgery. Now, they want me to visit their hospital next time we go. It was a very successful trip.”
What An didn’t know at the time was that she reportedly had performed the first MIGS procedure in all of India.
“I’m surprised they didn’t have that resource until now because we’ve been doing MIGS for 10 years in the United States, and we are seeing great results and so many patients benefit from this safe surgery,” An said. “I showed them what I do, and what works for us. It was such a beautiful exchange of knowledge and patient care.”
Joining An and Pimpalwar on the recent trip to India were Sumit Gupta, MD, associate professor of orthopaedic surgery; Kelly Scott, FNP; and Ben Burch, MD, resident physician.
An has already committed to joining the group again next year. She hopes to raise enough money to present Kasturba Hospital with a new surgical microscope – a token of her appreciation for the lessons she learned on her first ever humanitarian trip.
“Starting something new is always hard,” An said. “I really wanted to go but had a fear of the unknown. But I was so glad that I went. I felt like I learned so much more than what I was able to give.”
Read more
Against doc’s advice, parents pick male gender for child with sex disorder
Stanley Pinto
Feb 28, 2019, 4:59 ISTMangaluru : The decision of a city couple to assign male gender to their baby against the doctor’s advice has led to a debate in medical and social circles. Born with ambiguous sexual organs, the two-month-old baby has undergone surgery and will now be brought up as a boy.
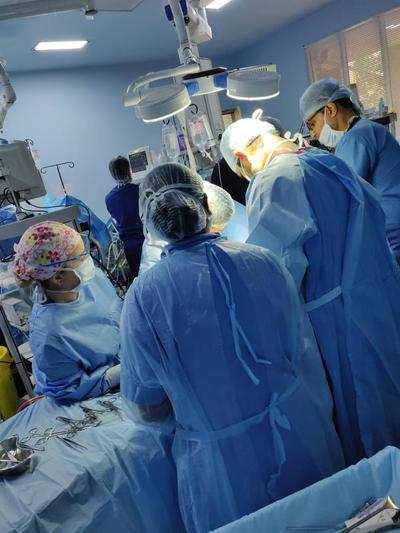
MGD is a common disorder of development (DSD) and is the second-most common cause of malformed sex organs.
The infant was born with vestigial sex organs and doctors suggested that the child would fare better as a female. Even if a phallus was created to make him male, they argued, there would be no real sense of manhood.
“The child was born with ambiguous genitalia. On the left side, the ovary was a little streak but there were no fallopian tubes. On the right, in the scrotum, there was some tissue like ovary and testes fused together,” Pimpalwar said. “Because there were no functional testes or ovaries and the internal organs of the child were rudimentary and like those of a female, we removed the organs and the ovaries because there could be risk of cancer.”
The parents were now faced with a dilemma – what should the gender of the child be? “It is better to bring up such a child as a female because it is difficult to fashion a functional phallus. The child will face psychological trauma when he grows up. So we suggested to the family that the child be brought up as a female. We could create a vagina as it was easier to do that,” said Pimpalwar. However, she would not be able to conceive on becoming an adult.
“We counselled the parents, who were well off, but they wanted a male child even if the imminent trauma would lead to suicidal tendencies,” said Pimpalwar.
Early February, in a five-hour operation, the child was given a neo-penis.
While Pimpalwar alleged that the well-off couple had made their choice for the love of a son in a patriarchal society. “In the US, there is an ethics committee for such cases when the patient or parent disagrees with the doctor. There is no such mechanism in India,” he said.
Social scientist Robert Da Silva disagreed. “A doctor at the operation table does not have the right to decide the sex of the child,” he said. “The talk of suicidal tendencies is unfounded as doctors cannot predict what behaviour the child may exhibit in future. The parents’ choice should be given preference since it is their child.”
Others felt it was a tough decision for the parents to make and might work in the long run.
“Now that the child has undergone the surgery, we have to wait and watch. Sexual inadequacy is a trauma, but it’s not killing,” said Dr SS Vasan, consultant andrologist at Manipal Hospitals.
“Since the surgery is done, the boy might get socially adjusted in future. However, due to the lack of an ethical committee and social service network, we can’t ascertain whether what’s being done is in the best interest of the child,” said Dr Karan Shetty, plastic surgeon at Sagar Hospitals.
Other medical experts TOI spoke to felt surgery could have waited for 4-5 years to allow the natural development of the child. “A chromosomal report of the child is essential to understand the genetic makeup. I’m surprised the baby withstood the major surgery at two months,” one of them said.
With inputs from Sunitha Rao in Bengaluru
Read more
Rebirth for kids with congenital anomalies
Chaitanya Deshpande
Feb 19, 2019, 3:59 ISTNagpur, : Samir Khiratkar, 15, from Ramtek used to look abnormal due to the S-shape curve in his spine. Suffering from scoliosis, Samir could not stand or walk normally till 2015. His mother Kalavati, who works as daily wager in a factory, could not afford any treatment for him and the boy had to suffer this medical condition for over 13 years.
“It was life changing moment for our family. We came here today to thank doctors coming from Germany who operated my son,” said his mother. She literally broke down while interacting with a senior nurse who was a part of the team that had performed surgery on Samir in 2017."
"They were at the Bal Shalyakriya Mission (paediatric surgery mission), a six-day surgery camp coordinated by US-based Charity group Peedh Parai International and Balmitra Foundation in Nagpur. The camp, into its six year, began at GMCH on Monday."
A 12-member team of expert paediatric surgeons from Germany, Switzerland and USA performed 18 specialized surgeries on the first day. Their target is to complete at least 75 surgeries by Saturday.
undefined
“We come to India every year for a week and offer services to kids suffering from congenital anomalies. We perform complicated surgeries on rare anomalies. Our team includes surgeons, anaesthesiologists, intensivists, specialist physicians, physician assistants, nurses and support personnel,” said Dr David Antekier who is paediatric orthopaedic specialist.undefined
undefined
Interestingly, chairman and founder of this organization, Dr Ashwin Pimpalwar, is from Nagpur. He is paediatric surgeon at Baylor College of Medicine, Houston, Texas. “Being GMCH alumni, I always wanted to do something here for my people. Unfortunately, many people in rural Vidarbha are not even aware that congenital anomalies can be treated with simple surgeries. Many kids live with the abnormality for years together. We screen such complicated cases through Balmitra Foundation and treat them for free,” he said. undefined
undefined
Balmitra Foundation is also run by a Nagpurian Dr Rajendra Saoji. undefined
undefined
On Wednesday, doctors are going to perform a surgery on a toddler for a very rare lung-related disorder. undefined
undefined
undefinedRead moreundefined
undefined
undefined undefined
Mangaluru: Dr H S Ballal inaugurates 3rd Bal Shalyakriya Mission Week
undefinedDaijiworld Media Network - Mangaluru (ANK)
Tue, Feb 5 2019 03:14:30 PMundefinedundefined
undefined Mangaluru, : Pro-chancellor of Manipal Academy of Higher Education Dr H S Ballal inaugurated the 3rd Bal Shalyakriya mission week here on Monday, February 4 at KMC Hospital, Attavar. Addressing the gathering, Dr H S Ballal said, "We need to support the needy which should be our ultimate responsibility. Programmes like these are a necessity. There are myriad numbers of people who are below poverty line and cannot afford medical expenses. In such cases we should help them.” undefined
undefined
undefined
undefined
Mangaluru south MLA Vedavyas Kamath said, "I congratulate KMC Hospital for taking up initiative in conducting the programme which is useful for poor. KMC has been giving quality treatment for people. Such programmes need to be organised by the government, but KMC has come forward to do it. In our district hospitals, enough facilities are not available for patients and KMC has been supporting the government in providing facilities in emergency cases.”undefined
undefined
Medical superintendent of KMC Hospital Dr Anand Venugopal welcomed the gathering.undefined
undefined
District health officer Dr Ramakrishna Rao, trustee Bantwal Ananth Mallya Charitable Trust Jeethendra Nayak, Dr Venkataraya Prabhu, dean, KMC and others were present.undefined
undefined
undefined
undefined
KMC Attavar to provide free Paediatric Surgical Treatment from Jan 16 to 25
undefinedUdayavani
January 18, 2017 05:33:39undefinedundefined
undefined Mangaluru, : On the occasion of completion of 25 successful years of providing clinical services, KMC Hospital at Attavar in Mangaluru is organising an advanced ‘Paediatric Surgical Treatment Week’. The treatment week will be organised under Bal Shalya Kriya Mission Mangaluru in collaboration with Peedh Parai Foundation, Houston (USA) and Bantwal Ananth Mallya Charitable Trust whereby children with untreated complicated surgical conditions which require very high surgical expertise will be treated free of cost by team of expert Pediatric Surgeons from Texas Children’s Hospital, Houston and KMC Hospital. undefined
undefined
undefined
undefined
Patients suffering with congrnital anomalies, Anorectal malformation, Hirschsprungs disease, Vesicoureteric reflux, Puj obstruction, Thoracic and Lung congenital anomalies etc. can take the benefits of this BSM week. All types of unattended, correction pediatric surgery cases will be treated free of cost by team of expert Paediatric Surgeons from Texas Children’s Hospital-Houston, USA and KMC Hospital Mangaluru.undefined
undefined
KMC Hospital Attavar, Mangaluru is first in Karnataka state and second in India to partner with Peedh Parai international and implement this social initiative for children.undefined
undefined
undefinedRead moreundefined
undefined
undefined undefined
Free Advanced Paediatric Surgical Treatment Week, Bal Shalyakriya Mission
undefinedPress Release
January 17, 2017undefinedundefined
undefined Mangaluru, : On occasion of completion of 25 successful years of providing clinical services KMC Hospital Attavar is organising an advanced Paediatric Surgical treatment week under Bal Shalya Kriya Mission Mangaluru in collaboration with Peedh Parai Foundation, Houston (USA) and Bantwal Ananth Mallya Charitable Trust whereby children with untreated complicated surgical conditions which require very high surgical expertise will be treated free of cost by team of expert Pediatric Surgeons from Texas Children’s Hospital, Houston, USA and KMC Hospital Mangaluru. undefined
undefined
undefined
undefined
Peedh Parai international is a non-profit organisation recognised worldwide with a renowned clinical team who are experts in advanced child related surgeries whereby children suffering and living with any treatable surgical conditions in different part of the world are treated free of cost.undefined
undefined
KMC Hospital Attavar, Mangaluru is First in Karnataka state and Second in India to partner with Peedh Parai international and implement this social initiative for children Patients suffering from congenital anomalies, Anorectal malformation, Hirschsprungs disease, vesicoureteral reflux, Puj obstruction, Thoracic and Lung congenital anomalies etc. can take the benefits of this BSM week.undefined
undefined
All types of unattended / correction pediatric surgery cases will be treated free of cost by a team of expert Paediatric Surgeons from Texas Children’s Hospital-Houston, USA and KMC Hospital Mangaluru.undefined
undefined
undefinedRead moreundefined
undefined
undefined undefined
Surgical camp brings hope to children
undefinedTHE TIMES OF INDIA
Feb 4, 2016, 04.19 AM ISTundefinedundefined
undefined Nagpur : Twelve-year-old Sameer Khiradkar has always been dreaming of captaining a navy ship. He wants to emulate one of his uncle who is in merchant navy. But Sameer's parents never dared to imagine their son even behind the steering wheel of a car as he was born with a crooked spine and couldn't sit or walk straight for more than half an hour due to associated pain and discomfort. undefined
undefined
undefined
undefined
"We could never in our life have saved 10-12 lakh for the surgery working in a ginning mill near Ramtek. City doctors had told us that the operation would cost somewhere that much. Now at least we can think of our son's dream coming true," said Kalavati, Sameer's mother.undefined
undefined
Dr David and Schannon Antekeier, orthopaedic surgeon couple from the Columbus Regional Hospital Georgia, who specialize in correcting spinal and limb deformities in children have already operated a few cases of kypho scoliosis (crooked or abnormal curvature of spine) and deformities caused due to cerebral palsy in the limbs in the camp. They told TOI the surgery was very complex and risky. It also required special anaesthesiologists. "It is great that the Globus Medical donated a number of implants we needed to fix up in the spine to straighten it, thanks to Dr Ashwin Pimpalwar of PPI who has brought us here," said Dr Antekeier.undefined
undefined
Other doctors in the 32 member team that would be operating 100 children in the camp also thanked Dr Pimpalwar, who is also from TCH and a Nagpurian. undefined
undefined
Mothers of Rawita Khaloo, a 16-year-old girl from Bonde village in Gadchiroli, has been operated for a complex gall bladder associated problem and one and half-year-old Laxmi Pinjare from Nara in city, operated for creating a rectal opening in right place by urosurgeons, cannot but thank their fate for getting this rare opportunity offered to them at the camp. They thank Dr Rajendra Saoji, the LMH paediatric surgeon who is a BMF patron too, Dr Amol Deshmukh of HERD Foundation, a copartner in the camp for holding screening camps in villages to select the child patients.undefined
undefined
Dr Eric Jones, paediatric urologist from TCH who has already performed surgeries on tens children in correction hypospadias, a condition in which the opening of the urethra is on the underside of the penis, instead of at the tip, told TOI about a relatively complex surgery related to the problem. He actually revised an earlier operation done to correct the defect but it didn't yield desired results. Jones used the tissue from the inside of the upper lips of the boy to create tube like structure and give shape to the penis in collaboration with plastic surgeons.undefined
undefined
Dr Binoy Chandy, ENT otolaryngologist relieved a boy of what his peers felt was ugliness of his face. The boy had a number of cysts protruding on his face. He used a cartilage bone as a graft from the ear in the surgery. Dr Sudha Pidani, a paediatric anaesthesiologist from TCH, said she was here with her team as such surgeries were always better done with a familiar team. "It is easier for the surgeons to communicate with the anesthesian if s/he is a familiar person," she said.undefined
undefined
Child life specialist Tori Vlek is a link between children and doctors. She communicates between children and doctors pre and post-operatively for better results. Paediatric nurse Carissa Chavez and emergency nurse Amanda Chavez are here specially because of Dr Pimpalwar's passion for treating children.undefined
undefined
In a Nutshell undefined
- undefined
- 32 Surgeons from USA, UK and Germany are performing different operations on 100 children to correct birth defects undefined
- undefined
- The team including a few paediatric nurses, counsellors have travelled on their own expenses and are operating free undefined
- undefined
- Camp has specialists from all fields of paediatric surgery undefined
- undefined
- The camp partners are planning to make the surgical camp for children an annual feature undefined
- undefined
- The defects include holes in diaphragm, blocked bile ducts, swelling on kidney, crooked backbone, urological problems like genitalia located at wrong places, children with different defects of thorax, orthopaedic, general, plastic, ENT or parts of digestive system undefined
- undefined
undefined
undefined
undefined
6-day surgical camp to correct defects in 100 kids
undefinedTNN
January 31, 2016, 8:09 IST undefinedundefined
undefined NAGPUR: The NKP Salve Institute of Medical Sciences (NKPIMS) and Lata Mangeshkar Hospital (LMH) will be organizing a six-day surgical camp from February 1 to 6 wherein a hundred children, born with various types of defect, will be operated upon. The surgeries will be done free of cost by a team of 32 doctors from USA, UK and Germany. undefined
undefined
undefined
undefined
Speaking to reporters about the camp Dr Rajendra Saoji, patron BMF, said that it is for the first time that so many foreign doctors, including those from Indian origin, will be conducting operations on children with various congenital (birth) defects or deformities.undefined
undefined
These 100 children were shortlisted after screening 300 children from across various parts of Vidarbha, adjoining districts of Chhattisgarh and Madhya Pradesh in last six months. The defects in children include holes in diaphragm, blocked bile ducts, swelling on kidney, crooked backbone, urological problems like genitalia located at wrong places, children with different defects of thorax, orthopaedic, general, plastic, ENT or parts of digestive system. Major surgeries include 35 urology problems, 25 digestive system problems, 6 crooked backbone problems. Patients with crooked backbone can’t sit or stand normally. undefined
undefined
All the surgeons will be travelling on their own expense and staying too on their own. Some doctors are bringing in certain expensive implants needed for surgeries free of cost. Dr Ashish Pipalwar — from Texas Children Hospital in Houston who originally hails from Nagpur of PPI — is coordinating the project,” said Dr Saoji. undefined
undefined
PPI is a voluntary group of medical professionals in USA who wish to serve and provide free surgical treatment to underprivileged children of developing countries. undefined
undefined
Madhur Maheshwari, BMF, Prasanna Gururaj (PPI), Dr Kajal Mitra, dean NKPSIMS, Dr Manisha Albal, associate professor, paediatric surgery, Jitendra Nayak, GSB Sabha, Dr Milind Bhrushundi, Medical Superintendent (LMH), Dr Subha Gade shared their views on the occasion. undefined
undefined
undefinedRead moreundefined
undefined
undefined



